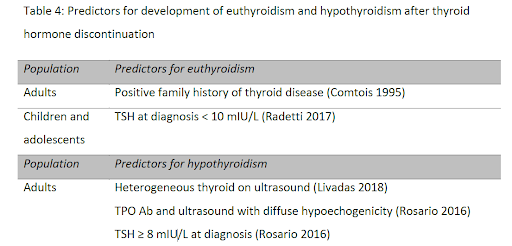
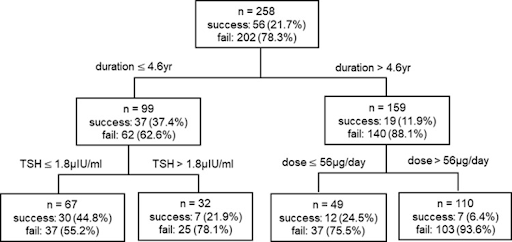
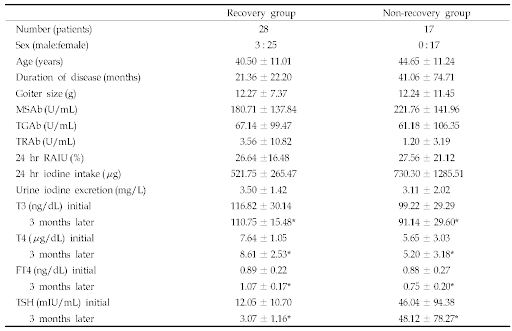
The study also shows that you’re less likely to respond to reducing your iodine intake alone if you have high TSH levels, had the disease for a long duration, or show more elevated anti-TPO antibodies.
Iodine and TPO
What is TPO, and how does it relate to iodine?
Lowering your iodine intake alone can improve your odds of successfully deprescribing. It can also improve your odds of reducing your thyroid peroxidase (TPO) antibodies.
TPO is an enzyme in your thyroid gland. It plays a crucial role in producing thyroid hormones. Thus, it’s the perfect marker to detect how your thyroid responds to treatment.
Some of the studies on deprescribing suggest that a higher TPO predicts an inadequate response, which is particularly true for people with heterogeneous or hypoechoic ultrasound findings.
So if you have a high TPO level, lowering your iodine intake may not be the answer for you.
Maintain Micronutrient Sufficiency
The one thing the studies I previously cited fail to evaluate is the participant’s micronutrient sufficiency. This includes vitamins and minerals.
Tons of data show that low levels of some micronutrients predict your thyroid disease may worsen.
The top micronutrients to focus on for thyroid health include:
- Selenium
- Zinc
- Vitamin D
- Magnesium
(Read More: Top 21 Nutrients for Optimal Thyroid Function).
The best course of action is to maintain these nutrients, which are more manageable by using a thyroid-specific multivitamin like my Daily Reset Packs rather than focusing on several isolated micronutrients.