From what we know, your thyroid needs iodine, so how is it possible that iodine could do it harm? This is a question I get all of the time, and I am more than happy to break it down for you in greater detail. So, let’s get to it.
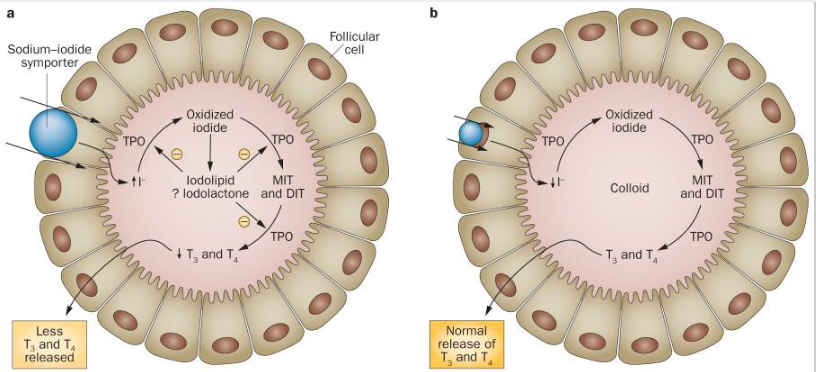
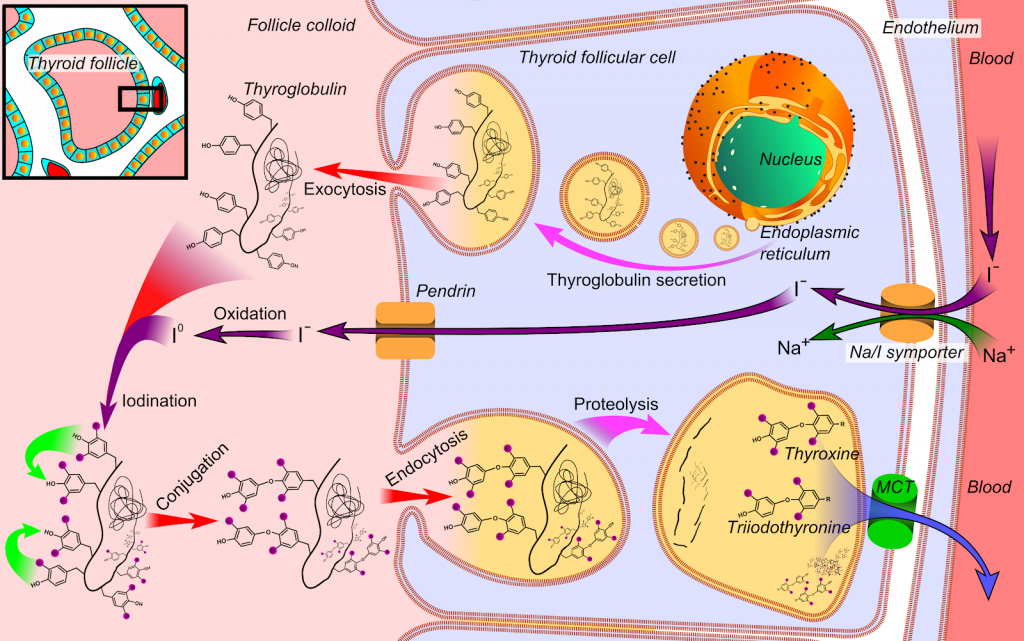
Let’s talk about the mechanisms by which we know it works, the evidence we have from studies of populations, and also some evidence we have from interventional trials. All of these line up to give us a really comprehensive overview of how iodine causes thyroid disease.
In fact, concerns about iodine factored heavily into creating my Ultimate Hypothyroid Bundle (Click Here: Learn more about this bundle today). It’s why everything I put together in there is conscious of iodine for your best health